What is Antibiotic Resistance?
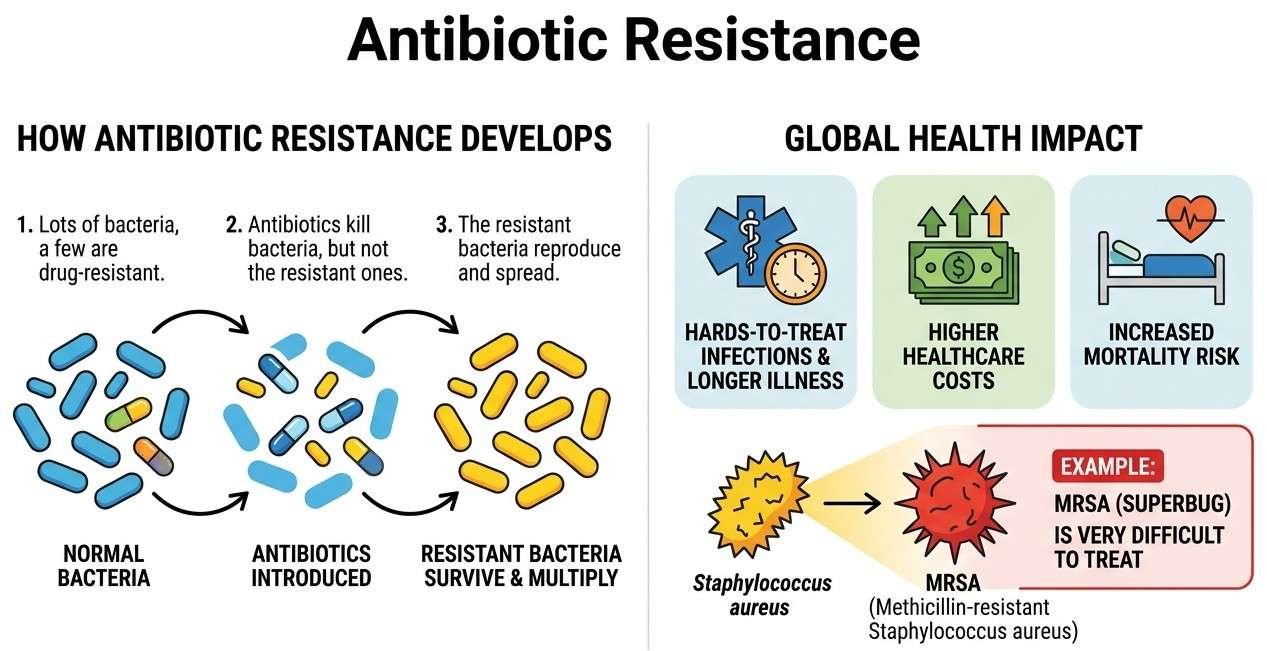
Antibiotic resistance is a serious global health problem where bacteria develop the ability to survive exposure to antibiotics that would normally kill them. This means infections become harder to treat, leading to prolonged illness, higher healthcare costs, and increased mortality.
For example, Bacteria like Staphylococcus aureus can develop resistance and turn into MRSA (Methicillin-resistant Staphylococcus aureus), which is much more difficult to treat.
Why Antibiotic Resistance is Dangerous?
Antibiotic resistance is a serious global health problem where bacteria develop the ability to survive exposure to antibiotics that would normally kill them. This means infections become harder to treat, leading to prolonged illness, higher healthcare costs, and increased mortality.
For example, bacteria like Staphylococcus aureus can develop resistance and turn into MRSA (Methicillin-resistant Staphylococcus aureus), which is much more difficult to treat.
1. Antibiotic Resistance: A Growing Public Health Crisis
- Antibiotic resistance is not just a scientific concern—it is a major public health crisis in the United States and worldwide.
- When bacteria become resistant, commonly used antibiotics lose their effectiveness, making even simple infections harder to treat.
- This leads to longer recovery times, increased hospitalization, and significantly higher healthcare costs.
- According to the World Health Organization, antibiotic resistance is one of the biggest threats to global health, food security, and development.
2. Why Antibiotics Are Losing Effectiveness
- One of the most serious risks is that minor infections can become life-threatening, especially when first-line antibiotics fail.
- Patients may require stronger, more expensive drugs with severe side effects, and in some cases, no effective treatment options remain.
- This is particularly dangerous in hospital settings, where healthcare-associated infections (HAIs) caused by resistant bacteria can spread rapidly among patients.
3. Impact on Surgeries, Chemotherapy, and Medical Procedures
- Antibiotic resistance also makes routine medical procedures more risky.
- Surgeries, chemotherapy, organ transplants, and even childbirth depend on effective antibiotics to prevent infections.
- Without reliable treatments, these procedures carry a much higher risk of complications and death.
- Additionally, resistant bacteria can spread quickly through communities via contact, food, water, and travel, turning local infections into widespread outbreaks.
4. Economic Burden on the U.S. Healthcare System
- Another critical issue is the increased burden on the U.S. healthcare system. Patients with resistant infections often require longer hospital stays, intensive care, and advanced treatments, which drive up medical expenses and strain hospital resources.
- This also leads to economic losses due to reduced productivity, as patients take longer to recover and return to work.
5. High-Risk Populations and Increased Mortality
- Vulnerable populations—including the people older than 70, children, and people with weakened immune systems—are at an even greater risk.
- For individuals with chronic conditions like diabetes or cancer, antibiotic resistance can lead to severe complications and higher mortality rates.
6. Threat to Modern Medicine and Urgent Action Needed
- In simple terms, antibiotic resistance threatens to push modern medicine backward, where common infections once again become deadly.
- Without urgent action, experts warn that resistant infections could cause millions of deaths annually, making it one of the most critical health challenges of our time.
Causes of Antibiotic Resistance
Understanding the causes of antibiotic resistance is essential for preventing its rapid spread. In the United States, the rise of drug-resistant bacteria (often called superbugs) is closely linked to how antibiotics are used in healthcare, agriculture, and the community. Below are the key factors contributing to this growing public health crisis.
1. Overuse of Antibiotics in Healthcare
- One of the leading causes of antibiotic resistance is the overprescription of antibiotics.
- In many cases, antibiotics are given when they are not needed, especially for viral infections like colds and flu, where they have no effect. This unnecessary exposure allows bacteria to adapt and develop resistance over time.
- In the U.S., studies have shown that a significant percentage of antibiotic prescriptions are avoidable. This misuse accelerates the emergence of antibiotic-resistant infections, making common treatments less effective.
2. Improper Use by Patients
- Even when antibiotics are prescribed correctly, improper usage by patients contributes significantly to resistance.
- Many people stop taking antibiotics once they feel better, rather than completing the full course. Others may take incorrect dosages or use leftover antibiotics without medical advice.
- This incomplete treatment allows some bacteria to survive and become stronger, leading to the development of multidrug-resistant organisms (MDROs).
3. Use of Antibiotics in Agriculture
- The use of antibiotics in livestock farming is another major contributor. In the U.S., antibiotics are often used not only to treat infections in animals but also to promote growth and prevent disease in crowded farming conditions.
- This practice encourages the development of resistant bacteria, which can spread to humans through food consumption, water contamination, and direct contact.
- As a result, agricultural antibiotic use plays a significant role in the global antimicrobial resistance (AMR) crisis.
4. Poor Infection Control in Healthcare Settings
- Hospitals and healthcare facilities can become hotspots for the spread of resistant bacteria if proper infection control measures are not followed.
- Poor hygiene practices, inadequate sterilization, and lack of proper isolation can lead to the transmission of dangerous pathogens.
- Infections acquired in hospitals, known as healthcare-associated infections (HAIs), are often caused by highly resistant bacteria, making them difficult and expensive to treat.
5. Lack of New Antibiotic Development
- Another critical issue is the slow development of new antibiotics.
- Pharmaceutical companies face high costs and regulatory challenges, resulting in fewer new drugs entering the market.
- As bacteria continue to evolve, the limited availability of new antibiotics creates a gap in treatment options.
- This makes it harder to combat emerging resistant strains and increases the risk of untreatable infections.

Mechanisms of Antibiotic Resistance
Bacteria don’t just “survive” antibiotics by chance—they use specific biological strategies to evade them. These antibiotic resistance mechanisms are the reason many infections in the United States are becoming harder to treat. Understanding how drug-resistant bacteria (superbugs) work is critical for developing effective therapies and improving infection control in healthcare settings.
1. Enzyme Production (Drug Inactivation)
- One of the most common mechanisms is the production of enzymes that break down or inactivate antibiotics before they can work.
- For example, some bacteria produce beta-lactamase enzymes that destroy penicillin-like drugs.
- This mechanism is widely seen in hospital pathogens and contributes to the rise of antimicrobial resistance (AMR) in the U.S., especially in healthcare-associated infections.
2. Efflux Pumps (Drug Removal System)
- Certain bacteria have specialized protein pumps called efflux pumps that actively push antibiotics out of their cells. This reduces the drug concentration inside the bacteria, making treatment ineffective.
- Efflux pump-mediated resistance is common in multidrug-resistant organisms (MDROs) and is a major concern in treating persistent infections.
3. Target Site Modification
- Antibiotics work by binding to specific targets inside bacterial cells.
- However, bacteria can alter these target sites, preventing the antibiotic from attaching and doing its job.
- This mechanism is responsible for resistance in many clinically important bacteria and is a key factor in treatment failure in infectious diseases across the United States.
4. Reduced Permeability (Blocking Drug Entry)
- Some bacteria develop resistance by reducing the permeability of their cell walls, which prevents antibiotics from entering the cell.
- This is especially common in Gram-negative bacteria, which already have a protective outer membrane.
- This mechanism contributes to the difficulty in treating infections caused by gram-negative superbugs in hospitals.
5. Biofilm Formation (Protective Shield)
- Bacteria can form biofilms, which are structured communities of microorganisms surrounded by a protective matrix.
- Biofilms act as a barrier, preventing antibiotics from reaching the bacteria effectively.
- Biofilm-associated infections are common in medical devices such as catheters and implants, leading to chronic infections and increased healthcare costs in the U.S.
Real-World Example
A well-known bacterium, Escherichia coli, can use multiple resistance mechanisms simultaneously—such as enzyme production and efflux pumps—making it a significant cause of antibiotic-resistant infections in both community and hospital settings.

Types of Antibiotic-Resistant Bacteria
Antibiotic resistance has led to the emergence of several high-risk, drug-resistant pathogens that pose a major threat to public health in the United States. These organisms—often referred to as superbugs—are responsible for many healthcare-associated infections (HAIs) and are difficult to treat with standard antibiotics. Understanding these key bacteria is essential for effective infection control, diagnosis, and treatment planning.
1. MRSA (Methicillin-Resistant Staphylococcus aureus)
- Staphylococcus aureus in its resistant form, known as MRSA, is one of the most well-known antibiotic-resistant bacteria in the USA. It is resistant to methicillin and several other commonly used antibiotics.
- MRSA infections can occur in hospitals (hospital-acquired MRSA) or in the community (community-acquired MRSA).
- It commonly causes skin infections, bloodstream infections, and pneumonia, and is a leading cause of hospital infections in the United States.
2. VRE (Vancomycin-Resistant Enterococci)
- Vancomycin-resistant Enterococci (VRE) are bacteria that have developed resistance to vancomycin, one of the last-resort antibiotics.
- These organisms are commonly found in hospital environments and primarily affect patients with weakened immune systems.
- VRE can cause serious infections such as urinary tract infections (UTIs), bloodstream infections, and wound infections, making them a major concern in infection control programs in U.S. hospitals.
3. MDR-TB (Multidrug-Resistant Tuberculosis)
- Multidrug-resistant tuberculosis (MDR-TB) is caused by strains of tuberculosis bacteria that do not respond to at least two of the most powerful anti-TB drugs.
- The bacterium Mycobacterium tuberculosis is responsible for this condition. MDR-TB requires long-term, expensive treatment with second-line drugs, and poses a serious challenge for public health systems worldwide, including the United States.
4. Drug-Resistant Mycobacterium tuberculosis
- In addition to MDR-TB, there are even more severe forms such as extensively drug-resistant TB (XDR-TB), where the bacteria become resistant to multiple classes of antibiotics.
- These infections are extremely difficult to treat and require specialized care.
- Drug-resistant TB is a major concern for global health security and infectious disease control, especially with increasing travel and migration.

Antibiotic Resistance in the USA
Antibiotic resistance has emerged as a major public health crisis in the USA, affecting millions of people every year. The rise of drug-resistant bacteria (superbugs) has made many infections harder to treat, leading to increased mortality, higher healthcare costs, and growing pressure on the medical system. As antimicrobial resistance (AMR) continues to evolve, it poses a serious threat to modern healthcare in the United States.
1. Rising Infections and Mortality
- In the United States, millions of antibiotic-resistant infections occur annually, with thousands of deaths linked directly to drug-resistant pathogens. These infections range from common illnesses like urinary tract infections to severe conditions such as sepsis and pneumonia.
- The increasing prevalence of multidrug-resistant organisms (MDROs) is making treatment more complex and less effective.
2. Healthcare-Associated Infections (HAIs)
- One of the biggest challenges is the spread of healthcare-associated infections (HAIs) in hospitals and clinical settings.
- Patients admitted for surgery, intensive care, or chronic illness are at a higher risk of acquiring infections caused by resistant bacteria.
- These infections often require longer hospital stays, advanced treatments, and higher medical expenses, significantly impacting both patients and healthcare providers.
3. Economic and Healthcare Burden
- Antibiotic resistance places a heavy burden on the U.S. healthcare system. Increased hospitalization, expensive second-line treatments, and prolonged recovery periods contribute to billions of dollars in healthcare costs each year.
- Additionally, productivity loss due to extended illness further affects the economy.
4. Infection Control and Prevention Measures
To combat this growing threat, hospitals in the United States are implementing strict infection control protocols. These include:
- Proper hand hygiene practices.
- Sterilization and disinfection procedures.
- Use of personal protective equipment (PPE).
- Isolation of infected patients.
Healthcare facilities are also adopting antibiotic stewardship programs, which promote the responsible use of antibiotics to reduce misuse and slow down resistance development.
5. Public Health Response in the USA
- Public health agencies are actively working to monitor and control antibiotic resistance through surveillance systems, research initiatives, and awareness campaigns.
- Efforts are focused on improving infection prevention strategies, encouraging appropriate antibiotic use, and developing new treatment options to address resistant infections.
Treatment Options for Antibiotic Resistance
Treating antibiotic-resistant infections is challenging, but with the right approach, many cases can still be managed effectively. In the United States, doctors use a combination of advanced therapies, targeted treatments, and supportive care to fight drug-resistant bacteria (superbugs). The goal is not only to eliminate the infection but also to reduce complications and improve patient outcomes.
1. Combination Therapy (Multi-Drug Approach)
- One of the most effective strategies is combination antibiotic therapy, where two or more antibiotics are used together.
- This approach increases the chances of killing resistant bacteria and reduces the likelihood of further resistance development.
- Combination therapy is commonly used in treating severe infections caused by multidrug-resistant organisms (MDROs) and is a key part of hospital infection treatment protocols in the USA.
2. Higher Dose Antibiotics (Optimized Dosing)
- In some cases, doctors may prescribe higher doses of antibiotics or adjust dosing schedules to achieve better results. This helps maintain an effective drug concentration in the body to combat resistant bacteria.
- However, this approach requires careful monitoring to avoid side effects and is typically used under strict clinical guidelines in U.S. healthcare settings.
3. New Antibiotics (Next-Generation Drugs)
- The development of new antibiotics is critical in the fight against resistance. Recent advancements have led to drugs specifically designed to target resistant strains of bacteria.
Although limited, these next-generation antibiotics are used in serious cases where standard treatments fail, offering hope for managing antimicrobial resistance (AMR).
4. Alternative Therapies (Innovative Treatments)
As resistance grows, alternative treatment options are gaining attention:
- Phage Therapy: Uses viruses to selectively kill bacteria.
- Immunotherapy: Enhances the body’s immune response to fight infections.
These innovative approaches are being researched and, in some cases, used in the USA to treat difficult infections caused by superbugs.
5. Supportive Care (Symptom Management)
Supportive care plays a vital role in recovery. This includes:
- Maintaining hydration.
- Managing fever and pain.
- Supporting immune function.
In severe cases, patients may require intensive care support, especially when infections lead to complications like sepsis.

Advanced Therapies (Future of Antibiotic Resistance Treatment)
As antibiotic resistance continues to rise, researchers in the United States are exploring next-generation therapies that go beyond traditional antibiotics. These innovative approaches aim to target drug-resistant bacteria (superbugs) more precisely, reduce treatment failure, and improve long-term outcomes. While many of these therapies are still under research or limited clinical use, they represent the future of antimicrobial resistance (AMR) treatment.
1. Phage Therapy (Bacteriophage Treatment)
- Phage therapy uses naturally occurring viruses called bacteriophages to infect and destroy specific bacteria.
- Unlike antibiotics, which can affect both harmful and beneficial bacteria, phages are highly targeted, making them effective against multidrug-resistant organisms (MDROs).
- This therapy is gaining attention in the USA for treating chronic and antibiotic-resistant infections, especially when conventional treatments fail.
- Ongoing clinical trials are evaluating its safety and effectiveness in modern healthcare settings.
2. CRISPR Technology (Gene-Targeted Therapy)
- CRISPR-based technology is a groundbreaking approach that allows scientists to edit bacterial DNA and directly target the genes responsible for antibiotic resistance. By disabling these resistance genes, CRISPR can make bacteria susceptible to antibiotics again.
- This advanced method is being explored as a potential solution for precision treatment of resistant infections and could revolutionize how we manage superbugs in the future.
3. Vaccines (Prevention Over Cure)
- Vaccination is one of the most effective ways to reduce the need for antibiotics. By preventing infections in the first place, vaccines help limit the spread of antibiotic-resistant bacteria.
- In the United States, vaccines play a key role in infection prevention strategies, especially for diseases that commonly lead to antibiotic use.
- Increased vaccination coverage can significantly reduce the burden of healthcare-associated infections (HAIs) and slow the development of resistance.

Prevention Strategies for Antibiotic Resistance
Preventing antibiotic resistance is the most effective way to protect public health and preserve the effectiveness of existing treatments. In the United States, reducing the spread of drug-resistant bacteria (superbugs) requires a combination of personal hygiene, responsible antibiotic use, and strong healthcare practices. These prevention strategies are essential for controlling the growing antimicrobial resistance (AMR) crisis.
1. Hygiene and Sanitation (First Line of Defense)
- Maintaining proper hygiene is one of the simplest yet most powerful ways to prevent infections.
- Regular handwashing with soap, keeping living and working environments clean, and following basic sanitation practices can significantly reduce the spread of harmful bacteria.
- Good hygiene not only prevents infections but also reduces the need for antibiotics, helping limit the development of antibiotic-resistant infections.
2. Responsible Antibiotic Use (Antibiotic Stewardship)
- Using antibiotics responsibly is critical in slowing resistance.
- Antibiotics should only be taken when prescribed by a qualified healthcare professional and should never be used for viral infections like colds or flu.
- Patients must also complete the full course of treatment, even if symptoms improve early. This approach, known as antibiotic stewardship, is widely promoted in the USA to reduce misuse and protect the effectiveness of existing drugs.
3. Infection Control in Hospitals
- Healthcare facilities play a key role in preventing the spread of resistant bacteria. Strict infection control protocols are essential to reduce healthcare-associated infections (HAIs).
- Key practices include:
- Proper sterilization and disinfection of medical equipment.
- Use of personal protective equipment (PPE).
- Isolation of infected patients.
- These measures are standard in U.S. hospitals to control the spread of multidrug-resistant organisms (MDROs).
4. Reducing Antibiotic Use in Agriculture
- The use of antibiotics in livestock farming contributes significantly to the spread of resistance. Limiting the use of antibiotics for growth promotion and disease prevention in animals is essential.
- In the United States, regulatory efforts are being made to reduce unnecessary antibiotic use in agriculture, helping control the spread of resistant bacteria through the food chain.
5. Vaccination (Preventing Infections Before They Start)
- Vaccination is a powerful tool in preventing infectious diseases and reducing the need for antibiotics. By lowering infection rates, vaccines help limit the emergence and spread of antibiotic-resistant pathogens.
- Routine immunization programs in the USA play a crucial role in infection prevention and public health protection.

Economic Impact of Antibiotic Resistance in the United States
Antibiotic resistance is not only a medical challenge but also a major economic burden on the U.S. healthcare system. The rise of drug-resistant infections leads to higher treatment costs, longer hospital stays, and increased demand for advanced medical care. As antimicrobial resistance (AMR) continues to grow, it is placing significant financial pressure on hospitals, patients, and the overall economy in the United States.
1. Increased Healthcare Costs
- Treating infections caused by antibiotic-resistant bacteria is far more expensive than treating non-resistant infections.
- Patients often require second-line or last-resort antibiotics, which are significantly more costly.
- In addition, the need for specialized diagnostics, extended care, and intensive monitoring increases overall medical expenses.
- In the USA, billions of dollars are spent annually on managing drug-resistant infections, making it a critical issue for healthcare policy makers and providers.
2. Longer Hospital Stays
- Patients with resistant infections typically experience longer hospitalization periods due to slower recovery and complications.
- Extended hospital stays not only increase costs but also raise the risk of acquiring additional healthcare-associated infections (HAIs).
- This creates a cycle where patients remain in healthcare facilities longer, further straining hospital resources and capacity.
3. Expensive and Complex Treatments
- Antibiotic resistance often requires the use of advanced and combination therapies, which are more expensive and may have stronger side effects.
- In some cases, patients need intensive care support, surgical interventions, or prolonged antibiotic courses.
- These complex treatments contribute to rising healthcare expenditures in the United States, especially in cases involving multidrug-resistant organisms (MDROs).
4. Productivity Loss and Economic Burden
- Beyond direct medical costs, antibiotic resistance also leads to loss of productivity. Patients may take longer to recover, resulting in missed workdays and reduced economic output.
- In severe cases, long-term disability or premature death further impacts families and the workforce.
- This indirect cost significantly adds to the overall economic burden of antimicrobial resistance in the USA.
5. Impact on the Healthcare System
- The growing prevalence of antibiotic resistance places immense pressure on the U.S. healthcare infrastructure. Hospitals must invest more in infection control, staff training, and advanced technologies to manage resistant infections effectively.
- Public health agencies are also increasing funding for research, surveillance, and prevention programs, further highlighting the economic scale of this issue.
Global Impact of Antibiotic Resistance
Antibiotic resistance is not limited to one country—it is a global health crisis that affects nations worldwide, including the United States. The rapid rise of drug-resistant bacteria (superbugs) has made infectious diseases harder to control across borders. As part of the growing antimicrobial resistance (AMR) threat, this issue requires coordinated international action to protect public health and ensure effective treatment options for future generations.
1. Affects All Countries and Healthcare Systems
- Antibiotic resistance impacts both developed and developing countries.
- From advanced healthcare systems in the United States to resource-limited settings, antibiotic-resistant infections are increasing everywhere.
- This widespread impact makes it a shared global challenge that affects hospitals, communities, and public health systems worldwide.
2. Spread Through Travel and Trade
- In today’s interconnected world, resistant bacteria can easily spread across borders through international travel, food supply chains, and global trade.
- A resistant infection acquired in one country can quickly appear in another, making containment difficult.
- This global movement contributes to the rise of multidrug-resistant organisms (MDROs) and highlights the importance of international surveillance and infection control strategies.
3. Need for Global Cooperation
- Addressing antibiotic resistance requires strong global collaboration between governments, healthcare organizations, and research institutions.
- Efforts include:
- Sharing data on resistant infections.
- Developing new antibiotics and therapies.
- Promoting responsible antibiotic use worldwide.
- Strengthening infection prevention programs.
- Organizations like the World Health Organization play a key role in coordinating international responses and setting global guidelines to combat antimicrobial resistance.

Why Awareness About Antibiotic Resistance is Important
Raising awareness about antibiotic resistance is one of the most effective ways to slow its spread and protect public health. In the United States, a lack of understanding about how antibiotics work—and when they should be used—continues to drive the rise of drug-resistant infections (superbugs). Educating individuals, patients, and healthcare providers is essential to reduce misuse and support better infection prevention strategies.
1. Reducing Misuse and Overuse of Antibiotics
- One of the biggest reasons for antibiotic resistance is the misuse and overuse of antibiotics.
- Many people still believe antibiotics can treat viral infections like colds or flu, which is incorrect.
- Increased awareness helps individuals understand that antibiotics should only be used when prescribed, supporting antibiotic stewardship programs in the USA.
- When people use antibiotics responsibly, it significantly reduces the chances of developing antibiotic-resistant bacteria.
2. Promoting Better Infection Prevention Practices
- Awareness campaigns encourage simple but powerful practices such as hand hygiene, sanitation, and vaccination. These steps reduce the spread of infections and lower the need for antibiotics in the first place.
- In healthcare settings, awareness among staff leads to better compliance with infection control protocols, helping prevent healthcare-associated infections (HAIs) caused by resistant bacteria.
3. Supporting Early Diagnosis and Proper Treatment
- Educated patients are more likely to seek timely medical care and follow treatment guidelines correctly.
- Awareness helps people understand the importance of early diagnosis, completing antibiotic courses, and avoiding self-medication.
- This reduces the risk of treatment failure and limits the spread of multidrug-resistant organisms (MDROs) in the community.
4. Encouraging Public Health and Policy Action
- Public awareness also drives policy changes and healthcare improvements. When communities understand the seriousness of antibiotic resistance, it increases support for research funding, surveillance programs, and stricter regulations on antibiotic use in healthcare and agriculture.
- Organizations like the World Health Organization actively promote awareness campaigns to combat the global antimicrobial resistance (AMR) crisis.
Conclusion
Antibiotic resistance is a growing global crisis that threatens to reverse decades of medical progress. Infections that were once easily treatable are becoming more dangerous due to the rise of drug-resistant bacteria, making routine treatments less effective and increasing the risk of complications, hospitalizations, and death.
The problem is driven largely by misuse and overuse of antibiotics, poor infection control, and the slow development of new drugs. However, it is also one of the few major health threats where human behavior can make a direct difference. Simple actions—like using antibiotics responsibly, maintaining hygiene, and supporting vaccination—can significantly reduce the spread of resistance.
Addressing antibiotic resistance requires a combined effort from individuals, healthcare providers, policymakers, and researchers. Strengthening antibiotic stewardship, improving infection prevention, and investing in new therapies are critical steps forward.
In the end, protecting the effectiveness of antibiotics is not just a medical responsibility—it is a shared global duty. The choices we make today will determine whether antibiotics remain powerful life-saving tools or become ineffective against future infections.
Frequently Asked Questions (FAQs)
Q1. What is antibiotic resistance?
Antibiotic resistance occurs when bacteria change in a way that allows them to survive antibiotic treatment. This makes infections harder to treat and increases the risk of disease spread, severe illness, and death.
Q2. What causes antibiotic resistance?
The main causes include overuse and misuse of antibiotics, not completing prescribed courses, using antibiotics for viral infections, and excessive use in agriculture. These factors allow bacteria to adapt and become resistant over time.
Q3. Why is antibiotic resistance a serious problem in the USA?
Antibiotic resistance is a major concern in the United States because it leads to millions of infections, thousands of deaths, and increased healthcare costs every year. It also makes routine medical procedures riskier due to infection complications.
Q4. Can antibiotic resistance be reversed?
In some cases, reducing antibiotic use can slow down resistance, but completely reversing it is difficult. Prevention and responsible antibiotic use are the most effective strategies to control its spread.
Q5. How can I prevent antibiotic resistance?
You can help prevent antibiotic resistance by:
- Taking antibiotics only when prescribed.
- Completing the full course of treatment.
- Avoiding self-medication.
- Practicing good hygiene (handwashing).
- Staying up to date with vaccinations.
Q6. Do antibiotics work against viral infections?
No, antibiotics are only effective against bacterial infections, not viral infections like colds, flu, or COVID-19. Misusing antibiotics for viruses contributes to resistance.
Q7. What are superbugs?
Superbugs are bacteria that have become resistant to multiple antibiotics, making them difficult to treat. These include infections caused by multidrug-resistant organisms (MDROs).
Q8. Who is most at risk of antibiotic-resistant infections?
People at higher risk include:
- Hospitalized patients.
- Elderly individuals.
- Children.
- People with weakened immune systems.
- Patients undergoing surgery or chemotherapy.
Q9. How does antibiotic resistance spread?
Antibiotic resistance spreads through:
- Person-to-person contact.
- Contaminated food and water.
- Poor hygiene and sanitation.
- Healthcare settings (hospital infections).
Q10. Are new treatments available for resistant infections?
Yes, new treatments such as advanced antibiotics, combination therapies, and alternative approaches like phage therapy are being developed. However, prevention remains the most effective solution.
Reference and Sources
- https://www.cdc.gov/narms/resistance
- https://infectioncycle.com/articles/mrsa-infections-causes-symptoms
- https://ourworldindata.org/antibiotics-livestock
- https://www.cdc.gov/antibiotic-use/data-research/facts-stats
- https://www.sir.advancedleadership.harvard.edu/articles/global-impact…
- https://www.scirp.org/pdf
- https://www.mdpi.com
Also Read
- Definition of General Medical Terms
- How Antibacterial Drug works?
- Bacillus thuringiensis (Bt): Complete Guide to Structure, Mechanism, Uses & Applications
- Application of Microbiology in Daily Life: Examples, Uses & Importance
- VDRL Test: Principle, Procedure, Interpretation, and Applications
- Helicobacter pylori: Morphology, Pathogenesis, Diagnosis, and Treatment
- Agriculture microbiology: Introduction, Function and interaction

