Pseudomonas aeruginosa– Etiology, Pathogenesis, and Treatment
Introduction
- There are diverse numbers of Pseudomonas species but P. aerugonisa is considered a clinically significant opportunistic pathogen.
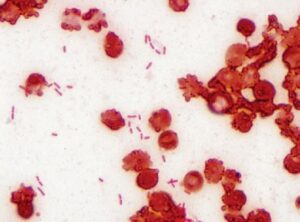
- P. aerugonisa are motile, aerobic, gram-negative rods,oxidase-positive, its bacteriologic characterization is the production of water-soluble pigments, few strains appear mucoid in presence of dense polysaccharides capsule.
Growth & Metabolism:
- It can be grown on simple media as it requires simple molecules like ammonia & CO2 for N2 and C requirements.
- Can survive on a wide variety of temperatures ranging from 20-42 °C and also in high salt concentration.
- In media, confluent growth (merged colonies), has a metallic sheen appearance, also the fruity odor is emitted.
- On blood agar, hemolysin is observed.
- Pigments are produced that are blue. yellow and rust in color, It helps to differentiate from other gram -ve rods.
- Blue pigment, Pyocyanin
- Yellow pigment, Fluorescin (fluoresces under UV light)
- Yellow-Green pigment, Pyoverdin
- Reddish Brown pigment, Pyorubin
Pathogenesis
- Virulence factors are associated with adhesins, toxins & enzymes which induce pathogenicity for Pseudomonas.
| Virulence Factors | Components of Virulence factors | Functions |
Adhesins |
|
|
Secreted Toxins and Enzymes |
|
|
Epidemiology
- Pseudomonas is ubiquitous in nature.
- It can grow in a diverse range of temperatures (4-42° C) with a minimum requirement.
- They are antibiotic-resistant due to porin mutation, which restricts the flow of antibiotic inside the cell; also produce enzymes to inactivates the antibiotics.
- They are opportunistic pathogens, usually, cause infection in burn patients.
Clinical Diseases
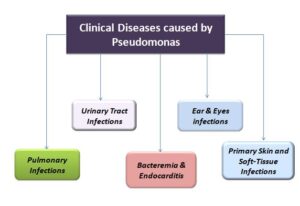
Pulmonary Infections
- Infects lower respiratory tract, may cause asymptomatic colonization, tracheobronchitis (benign inflammation of bronchial), and necrotizing bronchopneumonia (severe form).
- In cystic fibrosis patients, during Pseudomonas infections, mucoid strains are isolated.
- Characteristics of invasive disease caused by P. aeruginosa infections include bilateral bronchopneumonia with the formation of microabscess & tissues necrosis.
- The mortality rate is 70%.
Primary Skin and Soft-Tissue Infections
- P. aeruginosa causes various types of primary skin infections.
- Mostly recognized are burn wounds infections.
- Bacteria colonize the burn wounds, cause localized vascular damage, tissue necrosis, and bacteremia in severe cases of burn patients.
- The moist surface of the burn wound & failure in penetration of the neutrophils causes such infections.
- Only topical antibiotic creams are used for treatment in these cases.
- Folliculitis, caused by contaminated water( such as swimming pools, hot tubs) by Pseudomonas.
- Also, cause fingernails infections and osteochondritis (Bone & cartilage inflammation) of the foot can occur after penetrating injury (for e.g, stepping on a nail).
Urinary Tract Infections
- Cause in patients with long-term use of urinary catheters.
Ear Infections & Eye Infections
- Can cause swimmer’s ears infection (external otitis), it is managed by topical antibiotics & drying agents.
- In elderly & diabetic patients, P. aeruginosa can cause malignant external otitis, can invade the concealed tissues & damage cranial nerves & bones (fatal disease).
- Trauma in the eyes or abrasion from contact lens can cause infection.
- A more severe form like corneal ulcers can progress & can be fatal if not treated.
Bacteremia and Endocarditis
- Bacteremia occurs in patients suffering from extensive burns, diabetes mellitus, neutropenia( absence of neutrophils ).
- Originates from lower respiratory tracts, urinary tract, burn wound infections.
- Skin lesions (ecthyma gangrenosum) may develop, it can become ulcerated, hemorrhagic(vascular destruction) & necrotic.
- Endocarditis by pseudomonas is uncommon, but this condition is seen in intravenous drug abusers. ( Drug paraphernalia contaminated with waterborne organisms).
- It involves the tricuspid valve of the heart.
Laboratory Diagnosis
- Microscopy: Thin, gram-negative rods are observed arranged single or in pairs.
- Culture media: Selective isolation media is used, such as Blood Agar & MacConkey agar, it is identified by flat colonies with spreading border, pigmentation, colony size, hemolysis, and by rapid biochemical tests ( especially cytochrome oxidase-positive test).

Treatment
- Antibiotic therapy is not that effective due to antibiotic-resistant.
- Effective control practice of infections can be prevented by sterilizing equipment, such as dialysis machines & mechanical ventilation.
References and Sources
- https://quizlet.com/11628656/chapter-33-pseudomonas-and-related-bacteria-flash-cards/
- https://www.frontiersin.org/articles/10.3389/fmicb.2017.01566/full
- https://www.microbiologybook.org/Infectious%20Disease/Lower%20Respiratory%20Tract.htm
- https://www.infectiousdiseaseadvisor.com/home/decision-support-in-medicine/infectiousdiseases/
endocarditis-ivda/ - https://link.springer.com/chapter/10.1007/978-1-4614-0242-8_6
- https://bio.libretexts.org/Bookshelves/Microbiology/Microbiology_(OpenStax)/15%3A_Microbial_Mechanisms
_of_Pathogenicity/15.03%3A_Virulence_Factors - https://dermnetnz.org/topics/spa-pool-folliculitis/
